Introduction
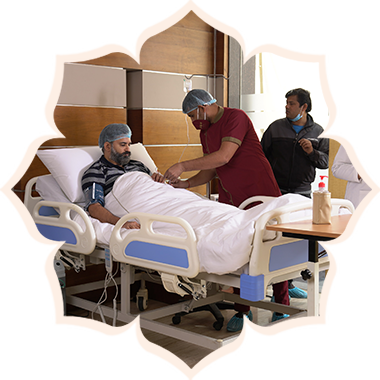
This case study highlights the recovery journey of a 56-year-old man who suffered a serious head injury after a construction site accident. He underwent traumatic brain surgery to remove blood clots and was later discharged with medical tubes and weaknesses on one side of the body. To support his recovery, he was admitted to Antara Care Home for close medical monitoring, nursing care, and physiotherapy.
Understanding the Case
-
Accident and Injury:
The patient is a 56-year-old man who met with a serious accident at a construction site. The impact caused severe head injuries, leading to bleeding inside the brain.
-
Medical Diagnosis:
Doctors found two types of brain bleeding extradural hematoma and subdural hematoma, which can be life-threatening if not treated quickly.
-
Emergency Brain Surgery:
He underwent decompressive craniotomy, a brain surgery done to remove the blood clots and reduce pressure on the brain. This surgery was crucial to save his life.
-
Condition After Hospital Discharge:
After surgery, he was discharged with:
- Reduced consciousness and difficulty following commands
- Feeding tube (Ryles tube) for nutrition
- Urinary catheter
- Weakness on one side of the body
- Agitation and restlessness
-
Need for Ongoing Care:
Due to his medical condition, he required 24/7 monitoring, nursing support, wound care, and physiotherapy. Managing such needs at home can be challenging for families.
Admission to Antara Care Home:
He was admitted to Antara Care Home for structured recovery, medical supervision, rehabilitation therapy, and support to improve his mobility and daily functioning.
Rehabilitation Approach
The patient
required a structured and step-by-step rehabilitation plan to support recovery
after brain surgery and prolonged hospitalization. The approach focused on
medical stability, physical recovery, and functional independence.
1. Medical
Stabilization and Monitoring
·
Continuous monitoring of vital signs and neurological status was done to
ensure the patient remained stable.
·
Regular wound checks and dressing were performed to prevent infection at
the surgical site.
·
Medications, including antibiotics and psychiatric medications, were
administered as prescribed to manage infection risk and agitation.
2. Behavioral and
Mental Health Support
·
In the early phase, the patient was irritable and agitated, which is
common after brain injury.
·
A psychiatrist’s consultation was taken, and appropriate medication was
started to calm agitation and improve sleep and behavior.
·
Supportive care and a calm environment helped reduce confusion and
restlessness over time.
3. Physiotherapy
and Mobility Training
·
Physiotherapy was initiated early to improve muscle strength and
movement in all limbs.
·
Gait training and assisted walking exercises were introduced to help the
patient regain balance and coordination.
·
Gradually, the patient progressed from assisted mobility to standing and
walking with minimal support.
4. Bladder and
Feeding Rehabilitation
·
Bladder training was started to restore natural urination, and the
urinary catheter was removed once safe.
·
Feeding support was provided initially through a feeding tube, and later
oral feeding was encouraged as the patient improved.
5. Infection and
Complication Management
·
Mild surgical site discharge and hematuria (blood in urine) were managed
with conservative treatment and antibiotics.
·
Regular assessments ensured complications were identified and treated
early.
6. Functional
Independence Training
·
Rehabilitation focused on helping the patient perform daily activities
like sitting, standing, and walking.
·
The long-term goal was to help the patient regain independence in daily
living activities with minimal support.
Outcome and Recovery Summary
With structured rehabilitation and medical care, the patient showed steady improvement over the weeks.
His agitation and irritability reduced significantly with psychiatric support
and medications. The surgical wound healed well, and infection was resolved
with timely treatment. Feeding improved from tube feeding to oral intake, and
bladder function was restored after catheter removal.
Physiotherapy
helped the patient regain strength and balance. He progressed from needing full
assistance to standing and walking with minimal support. By the end of the
rehabilitation phase, he was able to perform basic movements with supervision,
marking a positive step toward functional independence and improved quality of
life.
Communication Status
1. Early
Rehabilitation for Traumatic Brain Injury
Starting
physiotherapy and structured rehabilitation early helps traumatic brain injury patients
recover faster and prevent complications like muscle stiffness and weakness.
2. Behavioral
Changes Are Common After Brain Injury
Agitation,
irritability, and confusion are normal after brain trauma. Psychiatric support
and a calm environment can significantly improve behavior and mental
well-being. It requires 24/7 nursing care that Antara care homes provide to the
residents recovering from stroke, brain trauma or other conditions.
3. Medical
Monitoring Is Crucial After Discharge
Even after
hospital discharge, patients may need wound care, catheter care, feeding
support, and medication monitoring. Professional care settings can reduce risks
and stress for families.
4. Complications
Can Be Managed with Timely Care
Issues like wound
discharge or blood in urine can be treated effectively if detected early.
Regular assessments are key to preventing serious complications.
5. Recovery Is a
Step-by-Step Journey
Traumatic brain injury
recovery takes time. Small improvements—like sitting, standing, and walking are
major milestones that require patience, therapy, and consistent support.
6. Assisted
Living and Rehab Support Families
Structured rehab center provide 24/7 nursing, physiotherapy, and medical supervision, which can
be difficult to manage at home. This support helps families focus on emotional
care while professionals handle clinical needs.
Conclusion
A 56-year-old man suffered a severe head injury after a construction site accident and underwent emergency brain surgery to remove blood clots. After hospital discharge, he required feeding support, catheter care, wound management, and rehabilitation due to weakness, agitation, and reduced consciousness. He was admitted to Antara Care Home for structured medical monitoring and physiotherapy. With continuous nursing care, psychiatric support, infection management, and rehabilitation therapy, the patient showed steady improvement. He progressed from being agitated and dependent to standing and walking with minimal assistance, highlighting the importance of early rehabilitation and supervised recovery care.