Introduction
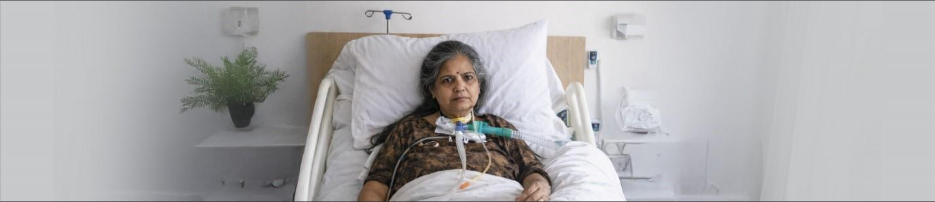
Life can change unexpectedly. For a 62-year-old female, what began as fever and severe neck pain soon turned into a serious neurological condition—Tuberculous Meningoencephalitis with Cerebral Venous Thrombosis. After undergoing a Mechanical Thrombectomy and later a Tracheostomy, she was left with severe weakness in all four limbs. Simple activities like sitting, standing, or moving became impossible.
Understanding the Case
This case study focuses on a 62-year-old female who developed a serious neurological condition, Tuberculous Meningoencephalitis, along with Cerebral Venous Thrombosis. The illness initially started with symptoms such as fever, neck pain, and body pain, but gradually affected her nervous system and physical functioning.
Due to the severity of neurological condition, doctors performed a Mechanical Thrombectomy to remove the clot and restore blood flow in the brain. Later, a Tracheostomy was also required to support her breathing during the critical phase.
After the medical procedures, the patient experienced Quadriparesis, meaning weakness in all four limbs. She struggled with basic movements such as turning in bed, sitting, standing, and walking, which normally happens in rehabilitation of patients with neurological deficit. Even simple daily activities like eating, grooming, or moving independently became extremely difficult.
Rehabilitation Approach
Rehabilitation Approach: Step-by-Step Recovery Journey
Recovering a severe neurological condition is not a single step but a gradual journey. For this 62-year-old female, neurological rehabilitation focuses on restoring functional independence through motor recovery and neuroplasticity. It aims to improve strength, balance, coordination, and daily living abilities. The goal is to enhance overall quality of life and reduce disability-one milestone at a time. It aims to improve strength, balance, coordination, and daily living abilities. The goal is to enhance overall quality of life and reduce disability-one milestone at a time.
Step 1: Protecting the Body and Preventing Complications
In the early stage, the patient had very limited movement due to severe weakness in all four limbs. Physiotherapy started with passive range of motion (PROM) exercises, gentle positioning, and chest physiotherapy to improve breathing and lung capacity. These early steps helped prevent bed sores, stiffness, and other complications while her body was still very weak.
Step 2: Encouraging Small Movements
As the body slowly responded, therapy progressed to assisted exercises (AAROM) where therapists helped her move her arms and legs. Breathing exercises continued to support lung function. Even small signs of movement were important milestones, giving the patient and her family hope that recovery was possible.
Step 3: Supporting Mobility and Sitting Balance
Once muscle tone began to improve, the focus shifted to bed mobility and sitting training. With support, the patient started practicing high sitting on the bed. A foot drop splint was used to support the ankles and maintain proper positioning. Wheelchair mobilization was also introduced to help her gradually adjust to upright positions.
Step 4: Standing with Support
With continuous therapy, muscle strength in both upper and lower limbs improved. The patient was able to stand with the help of two people and with the support of a foot drop splint. This was a significant emotional moment standing again after weeks of being unable to move independently.
Step 5: Beginning to Walk
Gradually, assisted walking was introduced. At first, the patient required support from two people. Over time, as muscle strength and balance improved, she progressed to walking with one person’s support. Each step represented progress not just physically but emotionally as well.
Step 6: Strengthening and Functional Training
As movement improved, therapy included active exercises (AROM) and strengthening using TheraBand, dumbbells, and weight cuffs. Core and back strengthening exercises were also introduced to improve posture, balance, and stability.
Step 7: Regaining Independence in Daily Life
With continuous post operative care at Antara Care Home, the patient gradually regained the ability to sit independently, walk with supervision, and perform daily activities. She was also able to practice stair climbing and ramp walking with assistance, bringing her closer to returning to a more independent life.
This step-by-step rehabilitation journey highlights how early physiotherapy, consistent care, and patient determination can lead to meaningful recovery even after severe neurological conditions like Tuberculous Meningoencephalitis and Cerebral Venous Thrombosis.
For the patient, every small improvement from moving a limb to taking the first steps became a powerful reminder that recovery is possible with the right support and right rehab centers.
Rehabilitation Goals
The rehabilitation plan for this 62-year-old female focused on gradual recovery, improving mobility, and helping her regain independence in daily life after Tuberculous Meningoencephalitis and Cerebral Venous Thrombosis. With structured neurological rehabilitation and regular physiotherapy, the goal was to restore strength, movement, and confidence.
Short-Term Rehabilitation Goals
- Enhance lung capacity and breathing through chest physiotherapy and breathing exercises.
- Initiate active or assisted movements.
- Prevent muscle atrophy.
- Improve muscle activation.
- Improve bed mobility such as turning and repositioning independently.
- Prevent complications like bed sores, joint stiffness, and muscle weakness.
- Begin assisted limb movements to support early neurological recovery.
Long-Term Rehabilitation Goals
- Achieve independent sitting balance without support.
- Improve muscle strength in both upper and lower limbs.
- Progress towards standing with support using assistive devices when required.
- Improve walking ability through gait training and physiotherapy.
- Build overall muscle strength, balance, and coordination.
- Help the patient become independent in daily activities (ADLs) such as sitting, standing, and moving safely.
- These rehabilitation goals were designed to support long-term recovery through structured physiotherapy, neurological rehabilitation, mobility training, and strength-building exercises, helping the patient gradually return to an active and independent life.
Conclusion
This case highlights how early and structured neurological rehabilitation can make a significant difference in recovery after severe conditions like Tuberculous Meningoencephalitis and Cerebral Venous Thrombosis. What began as a life-threatening illness that left a 62-year-old female unable to move or perform basic activities gradually transformed into a journey of steady recovery through consistent physiotherapy, strength training, and mobility rehabilitation.
With dedicated care and perseverance, the patient regained muscle strength, improved balance, and progressed from assisted movements to walking with supervision. This case demonstrates that with the right rehabilitation program, medical support, and patient determination, meaningful recovery and a return to independent daily life are possible.